This content is archived from the Feline Nutrition Foundation
Feline Inflammatory Bowel Disease: Nature and Treatment
- Updated: Sunday, April 28, 2019 05:04 PM
- Published: Friday, March 09, 2012 04:20 PM
- Written by Lyn Thomson, BVSc DipHom
 The inflammatory bowel diseases are the most common cause of chronic vomiting and diarrhoea in cats, and refer to a group of diseases. The term Inflammatory Bowel Disease, or IBD, is applied to a group of poorly understood gut pathologies that are considered to be a consequence of uncontrolled intestinal inflammation in response to a combination of elusive factors that may involve the diet, the environment, the gut microflora and dysregulation of the immune system in susceptible cats.
The inflammatory bowel diseases are the most common cause of chronic vomiting and diarrhoea in cats, and refer to a group of diseases. The term Inflammatory Bowel Disease, or IBD, is applied to a group of poorly understood gut pathologies that are considered to be a consequence of uncontrolled intestinal inflammation in response to a combination of elusive factors that may involve the diet, the environment, the gut microflora and dysregulation of the immune system in susceptible cats.
The main hypothesis for the cause and development of human IBD is that there is a dysregulation of the mucosal immune responses to intestinal microflora and/or dietary antigens.¹ This same abnormal immune response to dietary antigens is often suspected in feline IBD. Recent investigations have focused on attempts to better define the immunopathogenisis of the disease.²
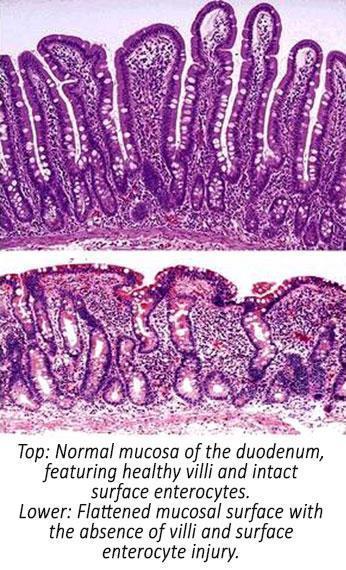 The absorption of digested food happens in the small intestine, mainly in the first two parts, the duodenum and the jejunum. The walls of these parts of the digestive system form tiny finger-like projections called villi with deep crypts between them. These villi are lined by cells called enterocytes, which work to absorb nutrients and pass them in to the blood stream to nourish the body. The importance of these cells can not be overstated. These cells are born in the base of the villi, known as the crypts, and travel to the top of the villi where they are shed off, constantly being renewed as in their short life, they work incredibly hard.
The absorption of digested food happens in the small intestine, mainly in the first two parts, the duodenum and the jejunum. The walls of these parts of the digestive system form tiny finger-like projections called villi with deep crypts between them. These villi are lined by cells called enterocytes, which work to absorb nutrients and pass them in to the blood stream to nourish the body. The importance of these cells can not be overstated. These cells are born in the base of the villi, known as the crypts, and travel to the top of the villi where they are shed off, constantly being renewed as in their short life, they work incredibly hard.
The changes seen in the intestines of a cat with IBD include clear architectural changes. The villi change their shape and become flat and blunted, fusing together and decreasing the surface area available for absorption of nutrients. Inflammatory infiltrate fills the crypts and flattens the wall of the gut. The cells lining the villi, the all important enterocytes, can no longer function properly. The integrity of the gut mucosa is damaged, and results in increased permeability to toxins from the gut lumen and increased bacterial translocation.
All of this damage leads to chronic vomiting and diarrhoea as the ability of the intestines to digest food is impaired.
Diagnosing IBD
The diagnosis of IBD requires the comprehensive exclusion of potential causes of gastrointestinal inflammation, including intestinal parasites, small intestinal bacterial overgrowth, bacterial enterocolitis, dietary intolerances and neoplasia.
To make a diagnosis of IBD, three features are normally present:
- A history of chronic gastrointestinal disease,
- Histopathological evidence of chronic inflammation of the gut with architectural changes to the gut,
- Exclusion of any known cause.
 A scoring system is in use in clinical practice for defining the severity and prognosis of IBD, known as the feline chronic enteropathy activity index.³ It grades cats on: their attitude and activity levels; appetite, from normal to severely decreased; frequency of vomiting, from none to more than three times per week; faecal quality, from normal to diarrhoea to faecal blood and mucus; degree of weight loss, from 0 to >10%; and also includes appearance of endoscopic lesions and total protein levels. The index is useful in assessing a cat's response to dietary change and treatment protocols.
A scoring system is in use in clinical practice for defining the severity and prognosis of IBD, known as the feline chronic enteropathy activity index.³ It grades cats on: their attitude and activity levels; appetite, from normal to severely decreased; frequency of vomiting, from none to more than three times per week; faecal quality, from normal to diarrhoea to faecal blood and mucus; degree of weight loss, from 0 to >10%; and also includes appearance of endoscopic lesions and total protein levels. The index is useful in assessing a cat's response to dietary change and treatment protocols.
Histopathological evidence is usually obtained by examining a sample of tissue from a biopsy of the cat's gut. Histopathological diagnosis is not straightforward, especially in cats, as the differentiation of lymphosarcoma and IBD can be difficult, if not impossible on a routine section.⁴ The surprising realisation in cats is that the prognosis for IBD may not be very different to the prognosis for lymphoma.⁵ A sequel to chronic IBD can be intestinal lymphoma. These tumours may occur because of the notorious habit of cats to develop tumours at sites of chronic inflammation.⁶
The Role of Gut Flora
The main purpose of having a digestive system is to be able to digest and absorb food. Without a healthy gut flora, the digestive system cannot fulfil this function. Anatomical integrity of the digestive tract, its functionality, ability to adapt and regenerate and ability to defend itself are directly dependent on the gut flora. It is established that the density and composition of the mucosal flora is related to the presence and severity of intestinal inflammation in cats, and suggests that mucosal bacteria are involved in the cause and development of feline IBD.⁷
 It is hypothesised that IBD could be a variable response to a specific pathogen or an inappropriate or excessive immunological response to normal luminal micro-organisms. The whole length of the digestive tract is coated with a tough bacterial layer providing a natural barrier against invaders, undigested food, toxins and parasites. These indigenous bacteria produce antibiotic-like substances, anti-funghal volatiles, anti-viral substances and they engage the immune system to respond appropriately to invaders. Without well-functioning gut flora the gut wall is unprotected and malnourished. Normal gut flora provides a major source of energy and nourishment for the cells lining the digestive tract.⁸
It is hypothesised that IBD could be a variable response to a specific pathogen or an inappropriate or excessive immunological response to normal luminal micro-organisms. The whole length of the digestive tract is coated with a tough bacterial layer providing a natural barrier against invaders, undigested food, toxins and parasites. These indigenous bacteria produce antibiotic-like substances, anti-funghal volatiles, anti-viral substances and they engage the immune system to respond appropriately to invaders. Without well-functioning gut flora the gut wall is unprotected and malnourished. Normal gut flora provides a major source of energy and nourishment for the cells lining the digestive tract.⁸
It is increasingly clear that dietary influences on the intestinal flora are involved in health and disease.⁹ It is likely that through interaction with the gut flora, certain diets could protect against the development of IBD whilst other diets actually predispose to the development of IBD. In the management of IBD it is prudent to select diets with a high digestibility. Information on the bioavailability of nutrients for cats and dogs is particularly lacking. The most commonly accepted methods of determining bioavailability of nutrients have not been validated for the cat.¹⁰
Diet and IBD
Let's look at diet as a trigger for IBD in cats. Our knowledge of nutrient requirements in cats is still incomplete, although a cat's basic nutrient requirements are amply present in the tissues of their prey animals. Most household cats no longer hunt but are instead fed commercially-prepared foods. These foods are rich in plant-derived nutrients because to supply cats with all-animal diets is seen as significantly more expensive. The trend has been to make foods with greater proportions of vegetable-based products and to supplement them with the necessary nutrients.¹¹
 The result is that the majority of cats are eating processed pet food containing poor quality, often inappropriate protein, grains, additives and preservatives, a far cry from the diet they are designed to eat. The pet food producers have recognised that many cats have food intolerances and food allergies, due in large part to the poor quality, biologically-inappropriate ingredients in commercial pet food, and the same manufacturers are now offering allergen-free varieties. The need for allergen-free pet food is the result of years of feeding poor quality protein, grains and fillers, toxic additives and preservatives to our obligate carnivores. A damaged gut will allow protein to trigger an allergic response.¹² Marketing claims identify protein as the primary culprit in food intolerances and specifically target intact animal protein. Hydrolysed protein diets are the current craze, the hydrolysed protein being small enough not to trigger an immune response. We need to recognise that the problem lies with the integrity of the gut wall. If we can repair the gut wall, the cat will no longer be intolerant of intact animal protein, the cat's natural diet.
The result is that the majority of cats are eating processed pet food containing poor quality, often inappropriate protein, grains, additives and preservatives, a far cry from the diet they are designed to eat. The pet food producers have recognised that many cats have food intolerances and food allergies, due in large part to the poor quality, biologically-inappropriate ingredients in commercial pet food, and the same manufacturers are now offering allergen-free varieties. The need for allergen-free pet food is the result of years of feeding poor quality protein, grains and fillers, toxic additives and preservatives to our obligate carnivores. A damaged gut will allow protein to trigger an allergic response.¹² Marketing claims identify protein as the primary culprit in food intolerances and specifically target intact animal protein. Hydrolysed protein diets are the current craze, the hydrolysed protein being small enough not to trigger an immune response. We need to recognise that the problem lies with the integrity of the gut wall. If we can repair the gut wall, the cat will no longer be intolerant of intact animal protein, the cat's natural diet.
The important point that seems to have been missed is that it is actually the feeding of a species-inappropriate diet that has led to the rise in inflammatory bowel disease in cats and loss of integrity of the gut wall.
By feeding cats inappropriately and not recognising them as obligate carnivores, we have damaged their intestinal tracts. We live in an era of convenience foods. Any processing of food changes its chemical and biological structure.¹³ The more food is processed, the more nutrient depleted and chemically altered it becomes. To compensate for the loss of taste, flavour and colour during processing, various chemicals are added including flavour enhancers, colours, various additives and preservatives. By negatively altering the gut flora, processed foods play an important part in damaging the intestinal tract. It is increasingly clear that dietary influences on the intestinal flora are involved in health and disease.¹⁴
Feeding your cat a species-appropriate diet, using a variety of protein sources in a highly digestible state, i.e. raw cat food, is the best way to avoid food intolerances and allergies.
Treating IBD – Using an Introduction Diet
It is my professional experience that a healthy balance of gut bacteria and a species-appropriate raw food for cats will protect and nourish the body. The introductory diet allows the gut lining to heal, restores the correct balance of intestinal bacteria and relieves the body of an excessive toxic load. Continuing to feed an appropriate raw cat food diet, once the gut has healed, is the best long term management of cats with IBD.
 Cats previously diagnosed with IBD may already be on steroids, and I would suggest that their medication be adjusted as improvement is seen. Steroids can be withdrawn slowly and many cats can be weaned off their medication, under the supervision of their veterinarian, by using the introductory diet, followed by a raw cat food diet.
Cats previously diagnosed with IBD may already be on steroids, and I would suggest that their medication be adjusted as improvement is seen. Steroids can be withdrawn slowly and many cats can be weaned off their medication, under the supervision of their veterinarian, by using the introductory diet, followed by a raw cat food diet.
Cats with serious digestive problems may show signs of diarrhoea, abdominal pain, bloating and constipation. These cats need to be transitioned to a raw diet via the introduction diet, which will reduce the symptoms quickly and initiate the healing process in the digestive system.
If it is not clear if the cat has IBD, food allergies or food intolerances, then the introductory diet is suggested in order to heal and seal their gut lining. The reason food allergies and food intolerances occur is due to what is called a "leaky gut," when the gut lining has been damaged by abnormal microflora.¹⁵ Foods do not get the chance to be digested properly before they get absorbed into the bloodstream through the damaged gut lining, and cause the immune system to react to them. Trying to identify which foods your cat reacts to is likely to be impossible. Foods leaked into the blood when only partially digested may cause an immediate reaction or a delayed reaction a day, a few days or even a couple of weeks later. As these reactions overlap, you can never be sure exactly what the cat is reacting to. Testing for food allergies is notoriously unreliable.¹⁶ As long as the gut wall is damaged and stays damaged, you can juggle the diet forever and get nowhere.
From my clinical experience, it is best to concentrate on healing the gut with an introductory diet. Once the gut wall is healed, foods will be properly digested before being absorbed, which will remove most food intolerances and allergies.
Introductory Diet of Homemade Meat or Fish Stock
Meat and fish stocks provide building blocks for the rapidly growing cells of the gut lining and they have a soothing effect on any areas of inflammation in the gut. Bone broth is rich in minerals including calcium, phosphorous, magnesium, sodium, potassium, sulphate and fluoride, all delivered in an easily-absorbable form. The minerals will improve immune function and support healthy digestion. Bone broth is also rich in collagen. Collagen is a protein containing two important amino acids, proline and glycine, and it will help heal the lining of the gut to relieve intestinal inflammation. Broths also contain glycosaminoglycans, also called GAGs, important building blocks for tissue repair.
This is why broths aid digestion and have been known for centuries as healing folk remedies for the digestive tract.¹⁷ Do not use commercially-available soup stock granules or bouillon cubes, as they are highly processed and contain detrimental ingredients such as MSG.
Chicken stock is particularly gentle on the stomach and is very good to start with. To make good meat stock, you need joints, bones, a piece of meat on the bone, a whole chicken, goose or duck, whole pigeons, pheasants or other inexpensive meats. It is preferable to use free range or organic meats when possible. It is essential to use bones and joints, as they provide the healing minerals and collagen, more so than the muscle meats.
If you are using larger-boned meats, ask the butcher to cut in half the large tubular bones, so you can get the bone marrow out of them after cooking. Put the bones, joints and meats into a large pan and fill it with water. Bring to boil, cover and simmer on a low heat for 2½ to 3 hours.
 You can make fish stock the same way using a whole fish or fish fins, bones and heads.
You can make fish stock the same way using a whole fish or fish fins, bones and heads.
After cooking, take the bones and meats or fish out and sieve the stock to remove small bones. Strip off all of the soft tissues from the bones as best as you can and encourage your patient to eat them. Reserve the extra for adding to meals later. Extract the bone marrow out of large tubular bones while they are still warm. To do that, bang the bone on a thick wooden chopping board. The gelatinous soft tissues around the bones and the bone marrow provide some of the best healing ingredients for the gut lining and the immune system; your patient needs to consume them with every meal.
The meat or fish stock will keep well in the fridge for at least seven days or can be frozen. Warm meat stock can be served to your cat at any time of day. Provide warm meat stock as a drink with meals and between meals.
It is very important for your patient to consume all of the fat in the stock and off of the bones, as these fats are essential for the healing process.
Probiotics are Essential to Introduce Right from the Beginning
Probiotics are found naturally in fermented foods, such as green tripe. For people, probiotics are found in foods such as kefir, sauerkraut and yoghurt. Probiotics provide a healthy balance of gut bacteria to protect and nourish the body.¹⁸ Probiotic bacteria ensure the gut is an effective first line of defence and ensure the effective digestion of food.
For cats, I use Bio-Kult® capsules. Some probiotics available in North America are Fortiflora®, Proviable®, Benebac® Plus and many brands made by smaller companies. Start with just a pinch on one meal a day, building to a pinch on every meal and in every drink of the broth. To avoid any reactions, introduce probiotic foods gradually.There can be a die-off reaction, which may present as lethargy in cats, as the body has to deal with the clearing of the bacteria which die off and any associated toxins they produce. A bit like a hangover/toxin overload. Make sure that the food is not too hot when adding the probiotic powder, as the heat will destroy the beneficial probiotic bacteria.
You can feed your cat more and more of the meat and soft tissues mixed with the broth until the signs of diarrhoea, bloating, abdominal pain and constipation have gone away. In most cats, this happens quite quickly, within a week or two, but in severe cases it can take months.
I would then introduce highly digestible species-appropriate raw cat food. In my practice, we usually start with rabbit fillets. We then progress to rabbit mince, which is ground meat, bone and organs. If fillets and mince are tolerated, we like to get cats chewing on pieces of raw meaty bone, such as rabbit shoulders, as quickly as possible. Introduce new raw foods regularly. Every week a new type of raw meat can be added, watching for any recurrence of clinical signs.
Additional Reading
Duke's Story: Inflammatory Bowel Disease
Feline Diabetes: The Influence of Diet
Saving Alistair: How Lyn Thomson Helped Stop IBD 11,000 Miles Away
The Keys to Improved Health
 What is important is that a cat has a healthy mucosal flora in the gut, and a species-appropriate diet. By optimising these two factors we give the cat the best chance of repairing the inflamed gut. So, a restorative diet and the restoration of the bowel flora are two key components of helping a cat with IBD.
What is important is that a cat has a healthy mucosal flora in the gut, and a species-appropriate diet. By optimising these two factors we give the cat the best chance of repairing the inflamed gut. So, a restorative diet and the restoration of the bowel flora are two key components of helping a cat with IBD.
There is a definite connection between the functioning of the gut and the functioning of the rest of the body.¹⁹ When food is not digested and absorbed properly, our cats suffer from multiple nutritional deficiencies. Inflamed guts become a source of toxins, rather than a source of nourishment. Healing and sealing the leaky gut is the key to improving health. The gut has great capacity for repair when fed a species-appropriate raw cat food diet.
Dr. Lyn Thomson trained at the University of Bristol in England and is studying with the Australasian College of Nutritional and Environmental Medicine. A dedicated and experienced advocate of bio-appropriate nutrition, Lyn practices in Auckland, New Zealand. HerRaw Essentialsstores have grown to seven retail locations, providing a variety of raw diet products for cats and dogs.
1. F Guarner, F Casellas, N Borruel, M Antolín, S Videla, J Vilaseca and JR Malagelada, "Role of Microecology in Chronic Inflammatory Bowel Diseases," European Journal of Clinical Nutrition no. 56, Supplement 4, Dec 2002, S34-8.
2. David Q Shih and Stephan R Targan, "Immunopathogenesis of Inflammatory Bowel Disease," World Journal of Gastroenterology, no. 14, vol. 3, January 21, 2008, 390-400.
3. AE Jergens, JM Crandell, R Evans, M Ackermann, KG Miles and C Wang, "A Clinical Index for Disease Activity in Cats With Chronic Enteropathy," Journal of Veterinary Internal Medicine no. 24, vol. 5, Sep-Oct 2010, 1027-33.
4. RJ Washabau, MJ Day, MD Willard, EJ Hall, AE Jergens, J Mansell, T Minami, and TW Bilzer, "Endoscopic, Biopsy, and Histopathologic Guidelines for the Evaluation of Gastrointestinal Inflammation in Companion Animals," Journal of Veterinary Internal Medicine, 2010, vol. 24, 10-26.
5. ML Wasmer, MD Willard, RG Helman and JF Edwards, "Food Intolerance Mimicking Alimentary Lymphosarcoma," Journal of the American Animal Hospital Association no.31, vol. 6, Nov-Dec 1995, 463-6.
6. Kevin N. Woodward, "Origins of Injection-Site Sarcomas in Cats: The Possible Role of Chronic Inflammation – A Review," International Scholarly Research Network Veterinary Science, vol. 2011, January, 17, 2011.
7. S Janeczko, D Atwater, E Bogel, A Greiter-Wilke, A Gerold, M Baumgart, H Bender, PL McDonough, SP McDonough, RE Goldstein and KW Simpson, "The Relationship of Mucosal Bacteria to Duodenal Histopathology, Cytokine mRNA, and Clinical Disease Activity in Cats with Inflammatory Bowel Disease," Veterinary Microbiology no. 128, vol. 1-2, April 1, 2008, 178-93.
8. BS Wostmann, "The Germfree Animal in Nutritional Studies," Annual Review of Nutrition vol. 1, July 1981, 257-279.
9. Emidio Scarpellini, Mariachiara Campanale, Diana Leone, Flaminia Purchiaroni, Giovanna Vitale, Ernesto Cristiano Lauritano and Antonio Gasbarrini, "Gut Microbiota and Obesity," Internal and Emergency Medicine vol. 5, supp. 1, Oct 2010, 53-56.
10. Jennifer A Larsen, C Christopher Calvert and Quinton R Rogers, "Processing of Dietary Casein Decreases Bioavailability of Lysine in Growing Kittens," Journal of Nutrition, supp. 132, June 2002, 1748S-1750S.
11. Angela G Glasgow, DVM; Nicholas J Cave, BVSc, MACVSc; Stanley L Marks, BVSc, PhD, Dip. ACVIM (Internal Medicine, Oncology), Dip. ACVN and Niels C Pedersen, DVM, PhD, "Role of Diet in the Health of the Feline Intestinal Tract and in Inflammatory Bowel Disease," Center for Companion Animal Health, School of Veterinary Medicine, University of California, Davis, CA.
12. WA Walker and IR Sanderson, "Epithelial Barrier Function to Antigens, An Overview," Annals of the New York Academy of Sciences, no. 664, October 1992, 10-17.
13. Jennifer A Larsen, C Christopher Calvert and Quinton R Rogers, "Processing of Dietary Casein Decreases Bioavailability of Lysine in Growing Kittens," Journal of Nutrition, supp. 132, June 2002, 1748S-1750S.
14. O Kanauchi, et. al., "Treatment of Ulcerative Colitis by Feeding with Germinated Barley Foodstuff: First Report of a Multicenter Open Control Trial," Journal of Gastroenterology, no. 37, supp. 14, Nov 2002, 67-72.
15. S Janeczko, D Atwater, E Bogel, A Greiter-Wilke, A Gerold, M Baumgart, H Bender, PL McDonough, SP McDonough, RE Goldstein and KW Simpson, "The Relationship of Mucosal Bacteria to Duodenal Histopathology, Cytokine mRNA, and Clinical Disease Activity in Cats with Inflammatory Bowel Disease," Veterinary Microbiology no. 128, vol. 1-2, April 1, 2008, 178-93.
16. WG Guilford, BR Jones, PJ Markwell, DG Arthur, MG Collett and JG Harte, "Food Sensitivity in Cats With Chronic Idiopathic Gastrointestinal Problems," Journal of Veterinary Internal Medicine, no. 15, vol. 1, Jan-Feb 2001, 7-13.
17. Barbara O Rennard, Ronald F Ertl, Gail L Gossman, Richard A Robbins and Stephen I Rennard, "Chicken Soup Inhibits Neutrophil Chemotaxis In Vitro," Chest, no. 118, vol. 4, October 2000, 1150-1157.
18. F Guarner, F Casellas, N Borruel, M Antolín, S Videla, J Vilaseca and JR Malagelada, "Role of Microecology in Chronic Inflammatory Bowel Diseases," European Journal of Clinical Nutrition no. 56, Supplement 4, Dec 2002, S34-8.
19. Emidio Scarpellini, Mariachiara Campanale, Diana Leone, Flaminia Purchiaroni, Giovanna Vitale, Ernesto Cristiano Lauritano and Antonio Gasbarrini, "Gut Microbiota and Obesity," Internal and Emergency Medicine vol. 5, supp. 1, Oct 2010, 53-56.




