This content is archived from the Feline Nutrition Foundation
Feline Pancreatitis: Signs of Trouble
- Updated: Saturday, June 01, 2019 05:59 PM
- Published: Saturday, September 06, 2014 08:21 PM
- Written by Guillermo Díaz. MV
 Pancreatitis can be a frustrating disease in cats. The cause often can't be definitively determined and the symptoms can be vague. Pancreatitis can range from low-grade with mild symptoms to severe, which can be fatal. Most often, treatment is supportive, alleviating symptoms and keeping the cat comfortable.
Pancreatitis can be a frustrating disease in cats. The cause often can't be definitively determined and the symptoms can be vague. Pancreatitis can range from low-grade with mild symptoms to severe, which can be fatal. Most often, treatment is supportive, alleviating symptoms and keeping the cat comfortable.
The pancreas is a lobulated gland located along a portion of the small intestine in mammals. The pancreas has two types of tissue, each synthesizing a different type of secretion. The exocrine portion, or acinar cells, produces enzymes utilized in the digestion of food. The endocrine portion, or islets of Langerhans, produces vital hormones such as insulin. Insulin is involved in the absorption and metabolism of glucose.
There are several diseases that can affect the normal functioning of the pancreas. In this article we're going to talk about inflammation of the pancreas, which is called pancreatitis. It happens when the enzymes produced and stored in the exocrine portion of the organ get activated inside it. This event causes the progressive autodigestion of the gland and the surrounding tissues. Normally, these digestive enzymes are encased in droplets while inside the pancreas and only become activated after travelling to the small intestine. It is the most common exocrine pancreatic disorder in cats.¹ Pancreatitis may be more common in cats than previously thought; a study that examined the pancreases of deceased cats found evidence of chronic pancreatitis in 45% of them.²
From the medical point of view, it is divided into two categories, acute pancreatitis and chronic pancreatitis, which is the more common of the two. Each has its own characteristics and clinical manifestations and each has different effects on the prognosis of the disease and the life of our patient. Both acute and chronic pancreatitis can cause scarring in the pancreas, which can impair its ability to function normally. Scarring can also affect the endocrine portion and insulin production, leading to diabetes.
The most common causes of pancreatitis in cats are:
- Damage to the pancreas from inflammation of the intestine
- Abdominal trauma
- Infectious diseases such as toxoplasmosis, FIP, herpesvirus or parasites
- Hepatic lipidosis
- Colangitis /colangiohepatitis
- Drugs such as phenobarbital, catabolic steroids and diuretics
- Ascending infections of small intestine³
 The association of pancreatitis with inflammatory bowel disease is frequently mentioned.⁴ One study found 30% of IBD cases to have histologic evidence of pancreatic involvement.⁵ Many cases of pancreatitis recognized with IBD have no specific clinical signs attributable to pancreatitis and should therefore be diagnosed as intestinal disease.⁶
The association of pancreatitis with inflammatory bowel disease is frequently mentioned.⁴ One study found 30% of IBD cases to have histologic evidence of pancreatic involvement.⁵ Many cases of pancreatitis recognized with IBD have no specific clinical signs attributable to pancreatitis and should therefore be diagnosed as intestinal disease.⁶
Although clinical signs are variable and non-specific, acute lethargy and anorexia are present in most of the cases.⁷ If your cat has a sudden episode of lethargy and is reluctant to eat, take her to the vet immediately. Clinical signs in cats with acute pancreatitis are:
- Lethargy
- Anorexia
- Dehydration
- Hypothermia
- Vomiting
- Abdominal pain
- Palpable abdominal mass
- Diarrhea
- Dispnea
- Weight loss
- Peritoneal effusion
- Jaundice
The diagnosis of feline pancreatitis can be challenging because the physical examination findings are non-specific, requiring a high amount of clinical suspicion and the combination of diagnostics tests.⁸
Your veterinarian will do hematology tests, also called blood work. The doctor will look for anemia, increased or decreased white cell count. Also, serum biochemistry will be performed to determine the levels of liver enzymes, bilirubin, cholesterol, urea and creatinine.
 The ordinary measurement of pancreatic enzymes such as lipase and amylase are not definitive for pancreatitis. For example, an increase in lipase levels only indicates a pancreatic pathology is present. This is the reason it must only be used as a screening test. More recently, better screening tests such as Spec fPL and Snap fPL have become available, although they are not always good at detecting mild pancreatitis. A combination of methods is a must.
The ordinary measurement of pancreatic enzymes such as lipase and amylase are not definitive for pancreatitis. For example, an increase in lipase levels only indicates a pancreatic pathology is present. This is the reason it must only be used as a screening test. More recently, better screening tests such as Spec fPL and Snap fPL have become available, although they are not always good at detecting mild pancreatitis. A combination of methods is a must.
Radiography usually only indicates that something abnormal is going on inside the abdomen. Pancreatitis is generally located in the "cranial part" of the cat's belly. Radiography may be useful in ruling out other possible causes of the symptoms, such as a bowel obstruction.
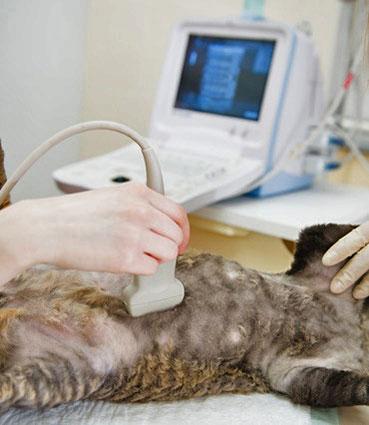
Ultrasound tests can sometimes see pancreatic abnormalities when performed by a skilled ultrasonographer, but not always. They may be useful in spotting concurrent problems in other organs such as the liver and intestines.
Definitive diagnosis can only be achieved by cytologic examination of pancreatic tissue. In other words, by doing a biopsy. Ultrasound-guided fine-needle aspiration of the pancreas is technically difficult due to the small dimension of this feline organ. Doctors may be very reluctant to perform biopsy of the pancreas because of the high risk of deleterious effects on the patient.⁹
The therapy for pancreatitis must address supportive care and the treatment, if possible, of the underlying cause. As a rule of thumb, treatment should include:

- Fluid therapy. Dehydration and electrolyte imbalances should be corrected within the first 12 to 24 hours.
- Pain management. Pain contributes to anorexia, and an anorectic cat may develop secondary conditions, such as hepatic lipidosis, that can worsen the prognosis.
- Nutritional support. Cats that have pancreatitis need careful nutritional support because in almost every case, they are inappetant.¹⁰ Lack of food can greatly increase the risk of concurrent hepatic lipidosis, making the situation even worse. Water should be reintroduced slowly, followed by small amounts of food. Some veterinarians recommend a low-fat diet, but high-fat diets are not viewed as a cause of pancreatitis.¹¹ Small, frequent feedings are preferable to large, single meals.¹² Enteral feeding may be needed temporarily for cats that will not eat.¹³
- Drug therapy. Antiemetics are frequently used in cats that are vomiting. Some drugs used in feline medicine for this purpose are dolasetron, ondansetron and maropitant.
Most cases begin as a sterile process, leading to controversy amongst clinicians concerning the use of antibiotics. When pancreatic necrosis occurs, the inflammatory process may predispose to bacterial colonization of the pancreas.¹⁴ The use of corticosteroids is of great help in cases of lymphocytic-type pancreatitis with or without concurrent IBD. Prednisolone given once or twice daily helps to reduce the inflammatory process. In cases of acute suppurative pancreatitis, the use of these drugs is contraindicated.
The prognosis for acute pancreatitis depends on the severity of the disorder and the presence of pancreatic and systemic complications such as pancreatic abscesses, infected necroses, pancreatic pseudocysts and especially hepatic lipidosis.¹⁵ Because many of these cats can be anorectic for prolonged periods of time, nutritional support has to be aggressive to prevent this often fatal complication.
Additional Reading
How Raw Food for Cats Affects Blood Test Results
Saving Alistair: How Lyn Thomson Helped Stop IBD 11,000 Miles Away
Cats with chronic pancreatitis may have damage or scarring of their pancreas and may not produce digestive enzymes in sufficient quantities. Additional digestive enzymes may need to be added as supplements. A caution about probiotics; a study in humans with pancreatitis associated the use of probiotics with a doubling of the risk of death.¹⁶ While this is not a study on cats, please discuss the use of probiotics with your veterinarian. Feeding a high-protein, palatable diet is critical – your cat must want to eat. A high-protein, low-carbohydrate diet is essential and raw cat food diets provide this high quality nutrition. Because IBD is frequently associated with pancreatitis, dealing with that underlying condition is beneficial. Work closely with your veterinarian on a diet that will be appropriate for your individual cat.
Dr. Guillermo Díaz and family, including their four dogs (Leroy, Xica, Moza and Pepa) and six cats (Michalina, Tigger, Vladimir, Yellow, Mongo and Chirusa) moved to Buenos Aires, Argentina in July of 2017, where he expects to continue supporting different animal rescue groups, spread the benefits of raw food for cats and dogs and write articles about nutrition.
1. JM Steiner, Small Animal Gastroenterology, Hannover, 2008.
2. HE De Cock, MA Forman, TG Farver and SL Marks, "Prevalence and Histopathologic Characteristics of Pancreatitis in Cats," Veterinary Pathology 44, no. 1, Jan 2007, 39-49.
3. S Little, The Cat: Clinical Medicine and Management, Elsevier Saunders, 2012.
4. DJ Weiss, JM Gagne and PJ Armstrong, "Relationship Between Inflammatory Hepatic Disease and Inflammatory Bowel Disease, Pancreatitis, and Nephritis in Cats," Journal of the American Veterinary Medical Association 209, no. 6, Sept 15, 1996, 1114-1116.
5. RM Baral, "Laparotomy for Gastro-intestinal Biopsies," Science Week Conference Proceedings, (Small Animal Medicine chapter), Gold Coast, Queensland, Australia, 2006, Australian College of Veterinary Scientists, p 70.
6. S Little, The Cat: Clinical Medicine and Management, Elsevier Saunders, 2012.
7. J Rand, Problem-Based Feline Medicine, Elsevier Saunders, 2006.
8. S Little, The Cat: Clinical Medicine and Management, Elsevier Saunders, 2012.
9. S Little, The Cat: Clinical Medicine and Management.
10. J Robertson, "Treating Feline Pancreatitis," DX Consult, vol. 2, no. 1, 2009.
11. J Robertson, "Treating Feline Pancreatitis."
12. CJ Gaskell, Feline Medicine and Therapeutics, Third Edition, Edited by EA Chandler, Blackwell Publishing, 2004.
13. J Robertson, "Treating Feline Pancreatitis," DX Consult 2, no. 1, 2009.
14. AL Widdison, C Alvarez, YB Chang, ND Karanjia and HA Reber, "Sources of Pancreatic Pathogens in Acute Pancreatitis in Cats," Pancreas 9, no. 4, July 1994, 536-541.
15. JM Steiner, Small Animal Gastroenterology, Hannover, 2008.
16. MGH Besselink, et al, "Probiotic Prophylaxis in Predicted Severe Acute Pancreatitis: A Randomised, Double-blind, Placebo-controlled Trial," The Lancet 371, no. 9613, Feb 2008, 651-659.




